SUN TEN Quarterly Newsletter Spring 2012: Two Cases of Thoracic Diseases with Clinical Results
Two Cases of Thoracic Diseases with Effective Clinical Results
by Dr. Jyh-Sheng You
Center for Traditional Chinese Medicine,

Forward
The thoracic diseases in this article refer to spontaneous pneumothorax and tuberculosis. Spontaneous pneumothorax is a commonly seen clinical emergency case of high incidence. Modern medicine uses thoracentesis to eliminate gas or surgical methods to cure or alleviate the condition. However, the recurrence rate is high. Traditional Chinese medicine refers to spontaneous pneumothorax as “chest pain” or “lung distention” and tuberculosis as “lung consumption”.
Tuberculosis is a consumptive disease caused by the contraction of tuberculin which corrode the lungs, cause chronic infection, and weaken the healthy Qi. The main clinical symptoms are coughing, coughing up blood, tidal fever, night sweat, and emaciation.
Case Study
[Case 1]
Mr. Chiu, a 42 year-old worker with a chief complaint of chest pain for one week, suffered difficult breathing when he moved as well as asthmatic coughing. He went to the emergency room at
Examination: The thorax was slightly asymmetric; the breathing sound in the right lung was clearly weakened and had a drum-like sound upon knocking. The left lung was normal. His tongue was red with a thick greasy yellow coating and slight teeth marks. His left pulse was slippery and rapid and his right pulse was wiry and rapid; yet when pressed deeply, it could not be felt. He was diagnosed with spontaneous pneumothorax and his disease pattern was differentiated as Qi and Yin deficiency with phlegm-heat harassing the interior. The treatment methods selected were to boost Qi, nourish Yin, and rectify Qi to dissolve phlegm.
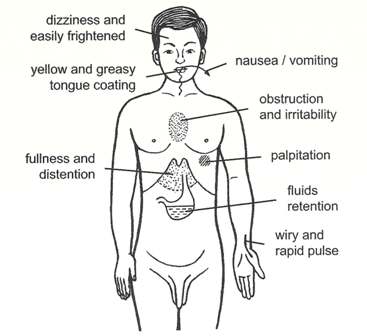
Pattern of Interior Disturbance of Phlegm-Heat
Prescription: TID for 7 days

After seven days, his symptoms weren’t clearly improved so he was referred to the Thoracic Surgery outpatient clinic for treatments. When the surgeon viewed his thoracic X-ray, a pulmonary resection was recommended. However, he refused it and returned to the TCM clinic.
Examination: It was discovered that his coughs were dry and he had right rib-side referring pain. His tongue was red and slightly dry with a thin, yellow coating. He still had a rapid pulse that could not be felt with deep pressure. The treatment methods were to boost Qi, nourish Yin, rectify Qi, and invigorate blood.
His symptoms were greatly improved after one week so he continued with the formula for another two weeks. A new thoracic X-ray showed that his right lung had completely opened up back to normal. We followed up after two years and his symptoms never relapsed.
Prescription: TID for 7 days
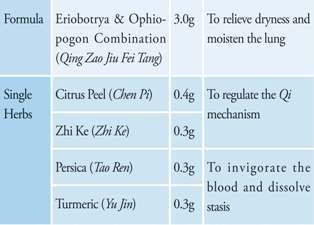
Join our member to get full-text article! Join Free!
[Case 2] for members only
[Diagnosis and Treatment Rational] for members only